-
Dyskinesia
Wikipedia
The symptoms include tremors and writhing movements of the body and limbs, and abnormal movements in the face, mouth, and tongue – including involuntary lip smacking, repetitive pouting of the lips, and tongue protrusions. [11] Rabbit syndrome is another type of chronic dyskinesia, while orofacial dyskinesia may be related to persistent replication of Herpes simplex virus type 1 . [12] Non-motor [ edit ] Two other types, primary ciliary dyskinesia and biliary dyskinesia , are caused by specific kinds of ineffective movement of the body, and are not movement disorders . ... External links [ edit ] Classification D ICD - 10 : G24.9 ICD - 9-CM : 333.8 MeSH : D020820 DiseasesDB : 17912 SNOMED CT : 9748009 External resources Patient UK : Dyskinesia v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis v t e Symptoms and signs relating to movement and gait Gait Gait abnormality CNS Scissor gait Cerebellar ataxia Festinating gait Marche à petit pas Propulsive gait Stomping gait Spastic gait Magnetic gait Truncal ataxia Muscular Myopathic gait Trendelenburg gait Pigeon gait Steppage gait Antalgic gait Coordination Ataxia Cerebellar ataxia Dysmetria Dysdiadochokinesia Pronator drift Dyssynergia Sensory ataxia Asterixis Abnormal movement Athetosis Tremor Fasciculation Fibrillation Posturing Abnormal posturing Opisthotonus Spasm Trismus Cramp Tetany Myokymia Joint locking Paralysis Flaccid paralysis Spastic paraplegia Spastic diplegia Spastic paraplegia Syndromes Monoplegia Diplegia / Paraplegia Hemiplegia Triplegia Tetraplegia / Quadruplegia General causes Upper motor neuron lesion Lower motor neuron lesion Weakness Hemiparesis Other Rachitic rosary Hyperreflexia Clasp-knife responseDRD2, OPRM1, PDYN, HTR2A, PPP1R1B, MYORG, CP, HTR1B, SLC2A1, SLC6A3, LRRK2, ADCY5, PNKD, PRRT2, GRIN2B, EEF1A2, GCDH, PDE10A, UBA5, SNCA, PINK1, FOXG1, KCNMA1, KCNA1, SLC1A2, WARS2, PRKRA, CACNA1B, GRIN2D, KCNQ2, CACNA1A, AARS1, TSPEAR, TSPEAR-AS1, STXBP1, SURF1, SYT1, TGFBR2, INPP5K, WWOX, CDKL5, SCN8A, ST3GAL3, VPS35, PRKN, SEMA4A, PDGFB, PIGC, PIK3CA, C12orf4, FMN2, PMS1, PMS2, PODXL, PPP3CA, VPS13C, LINS1, NSUN2, CC2D1A, APTX, RPS20, CLIP1, SARS1, SCN2A, SCN3A, ACTL6B, UCHL1, PRSS12, RSRC1, CUX2, DCPS, MAN1B1, PNKP, PARK7, CNKSR2, HTRA2, TRAK1, FAN1, TNIK, MLH3, DNAJC13, SLC45A1, WASHC4, SZT2, ATP13A2, SLC39A14, CYFIP2, FRRS1L, ATXN10, NDUFAF3, PARS2, NECAP1, KDM5B, DEAF1, EZR, ST3GAL5, XK, YWHAG, TUSC3, AP3B2, NTRK2, CASK, STX16, CRADD, SYNGAP1, SYNJ1, PIGP, SLC30A9, CRBN, PIGQ, MECR, AIMP1, MED23, TECR, SEPSECS, DNAJC6, SCO2, NDUFA13, WIPI2, SIL1, ARV1, HNMT, PNPT1, FTL, GABRB2, GABRB3, GABRG2, B4GALNT1, GBA, TRAPPC9, MED25, NEUROD2, GNAS, TRIM8, LMAN2L, GRIK2, GRIN1, EDC3, PGAP1, DHDDS, MSH6, FGF12, EIF4G1, SLC46A1, CLTC, AGA, HCN1, SLC13A5, ATP1A3, ATP6V1A, BMPR1A, CAMK2B, ARX, SPATA5, NUS1, SIK1, CSTB, DDX3X, B3GALNT2, DNAJC19, DNM1, METTL23, RAB39B, ZC3H14, GNAO1, GIGYF2, NDUFB8, NDUFS2, ATP6, TRNK, MSH2, MLH1, TRNV, NDST1, ND1, EPCAM, NDUFS4, MBOAT7, ND2, TRNL1, TMEM43, SLC25A22, KRAS, NDUFS8, ND3, ND4, KCNQ3, ND5, ND6, KCNB1, KCNA2, FBXO31, TRNW, COMT, DRD3, BDNF, GCH1, MCF2L, LRP2, GRM5, TH, DRD1, MAOB, PENK, ANKK1, REM1, CYP2D6, ADORA2A, TSEN54, PAFAH1B1, APOE, PDC, ASXL1, SF3B1, SOD2, MTOR, YWHAE, ATXN2, RGS9, MAPK1, TET2, FGF14, PRKD1, EPHB2, PRKCB, PRKCA, HOMER1, MEF2C, GPR88, BDNF-AS, MIR543, ATP8A2, PDIK1L, THAP1, TWNK, HEXD, DNER, C9orf72, STX1B, SBNO1, SHBG, RASD2, DRD4, ECHS1, EMD, FOSB, FOSL2, FSHMD1A, GAD1, GDNF, GFAP, GRK6, GPX1, GRIN2A, GRM4, GSTP1, HLA-A, NR4A1, TOR1A, DPP6, LAMC2, DNMT1, ACHE, GRK3, ALDH1A1, ARRB2, CA8, CACNA1E, CASP1, CD5L, CD69, CHRNA4, CNR1, CSF2, CST3, NQO1, DLG4, HTR2C, LMNA, ARC, SKIL, SRC, TNF, TPI1, TRH, UCP2, VEGFA, NOL3, TAAR5, LGI1, KMT2B, SIGMAR1, OGA, CIT, RPH3A, SBNO2, SPN, AOC1, LY6E, SGCA, MAOA, NOS3, OPRL1, SERPINA5, PITX2, PMCH, PNOC, POLG, POMC, PPP4C, MAPK3, PRSS2, PTN, PTPN11, RENBP, LOC107987479
-
Akinetic Mutism
Wikipedia
Other causes of akinetic mutism are as follows: Respiratory arrest and cerebral hypoxia [6] Acute cases of encephalitis lethargica [3] Meningitis [3] Hydrocephalus [3] Trauma [3] Tumors [3] Aneurysms [3] Olfactory groove meningioma Cyst in third ventricle [1] Toxical lesions and infections of central nervous system [10] Delayed post-hypoxic leukoencephalopathy (DPHL) [6] Creutzfeldt–Jakob disease (mesencephalic form) [2] Diagnosis [ edit ] Akinetic mutism can be misdiagnosed as depression , delirium , or locked-in syndrome , all of which are common following a stroke. [3] Patients with depression can experience apathy, slurring of speech, and body movements similar to akinetic mutism. Similarly to akinetic mutism, patients with locked-in syndrome experience paralysis and can only communicate with their eyes. [3] Correct diagnosis is important to ensure proper treatment. ... After eight months of rehabilitation, Elsie no longer experienced headaches or akinetic mutism symptoms. [1] See also [ edit ] Selective mutism Locked-in syndrome Athymhormic syndrome Catatonia Aboulia References [ edit ] ^ a b c d e f g h i j Cairns, H; R.
-
Progressive Vaccinia
Wikipedia
PMID 9086127 . v t e Skin infections , symptoms and signs related to viruses DNA virus Herpesviridae Alpha HSV Herpes simplex Herpetic whitlow Herpes gladiatorum Herpes simplex keratitis Herpetic sycosis Neonatal herpes simplex Herpes genitalis Herpes labialis Eczema herpeticum Herpetiform esophagitis Herpes B virus B virus infection VZV Chickenpox Herpes zoster Herpes zoster oticus Ophthalmic zoster Disseminated herpes zoster Zoster-associated pain Modified varicella-like syndrome Beta Human herpesvirus 6 / Roseolovirus Exanthema subitum Roseola vaccinia Cytomegalic inclusion disease Gamma KSHV Kaposi's sarcoma Poxviridae Ortho Variola Smallpox Alastrim MoxV Monkeypox CPXV Cowpox VV Vaccinia Generalized vaccinia Eczema vaccinatum Progressive vaccinia Buffalopox Para Farmyard pox : Milker's nodule Bovine papular stomatitis Pseudocowpox Orf Sealpox Other Yatapoxvirus : Tanapox Yaba monkey tumor virus MCV Molluscum contagiosum Papillomaviridae HPV Wart / plantar wart Heck's disease Genital wart giant Laryngeal papillomatosis Butcher's wart Bowenoid papulosis Epidermodysplasia verruciformis Verruca plana Pigmented wart Verrucae palmares et plantares BPV Equine sarcoid Parvoviridae Parvovirus B19 Erythema infectiosum Reticulocytopenia Papular purpuric gloves and socks syndrome Polyomaviridae Merkel cell polyomavirus Merkel cell carcinoma RNA virus Paramyxoviridae MeV Measles Togaviridae Rubella virus Rubella Congenital rubella syndrome ("German measles" ) Alphavirus infection Chikungunya fever Picornaviridae CAV Hand, foot, and mouth disease Herpangina FMDV Foot-and-mouth disease Boston exanthem disease Ungrouped Asymmetric periflexural exanthem of childhood Post-vaccination follicular eruption Lipschütz ulcer Eruptive pseudoangiomatosis Viral-associated trichodysplasia Gianotti–Crosti syndrome
-
Transposition Of The Great Vessels
Wikipedia
External links [ edit ] Classification D ICD - 10 : Q20.3 ICD - 9-CM : 745.1 OMIM : 608808 MeSH : D014188 DiseasesDB : 13259 External resources MedlinePlus : 001568 eMedicine : ped/2548 Patient UK : Transposition of the great vessels v t e Congenital heart defects Heart septal defect Aortopulmonary septal defect Double outlet right ventricle Taussig–Bing syndrome Transposition of the great vessels dextro levo Persistent truncus arteriosus Aortopulmonary window Atrial septal defect Sinus venosus atrial septal defect Lutembacher's syndrome Ventricular septal defect Tetralogy of Fallot Atrioventricular septal defect Ostium primum Consequences Cardiac shunt Cyanotic heart disease Eisenmenger syndrome Valvular heart disease Right pulmonary valves stenosis insufficiency absence tricuspid valves stenosis atresia Ebstein's anomaly Left aortic valves stenosis insufficiency bicuspid mitral valves stenosis regurgitation Other Underdeveloped heart chambers right left Uhl anomaly Dextrocardia Levocardia Cor triatriatum Crisscross heart Brugada syndrome Coronary artery anomaly Anomalous aortic origin of a coronary artery Ventricular inversionCFC1, GDF1, CFC1B, DVL2, TBX1, HSPG2, MED13L, ZIC3, GPC3, RAB23, PHGDH, NODAL, LMNA, CERS1, ZMPSTE24, PIGL, WT1, GJA8, GJA5, GATA6, NKX2-6, GATA4, GPC4, FKTN, FANCB, CFAP53, PKD1L1, CHD7, NKX2-5, BMP2, CGA, HAP1, MED12, CDC73, MED13, MED30, PDE5A, DICER1, MOCOS, FOXH1, ACVR2B, MKKS, TSC1, APEX1, BDNF, CECR, COL11A2, COX8A, DNMT1, DNMT3A, ERBB2, HIF1A, HOXA1, INSIG1, PHEX, PARP1, S100A1, S100B, TGFB1, TGM2, PITX2
-
Nonunion
Wikipedia
External links [ edit ] AAOS Classification D ICD - 10 : M84.1 , M96.0 MeSH : D005599 Wikimedia Commons has media related to Pseudarthrosis . v t e Bone and joint disease Bone Inflammation endocrine : Osteitis fibrosa cystica Brown tumor infection : Osteomyelitis Sequestrum Involucrum Sesamoiditis Brodie abscess Periostitis Vertebral osteomyelitis Metabolic Bone density Osteoporosis Juvenile Osteopenia Osteomalacia Paget's disease of bone Hypophosphatasia Bone resorption Osteolysis Hajdu–Cheney syndrome Ainhum Gorham's disease Other Ischaemia Avascular necrosis Osteonecrosis of the jaw Complex regional pain syndrome Hypertrophic pulmonary osteoarthropathy Nonossifying fibroma Pseudarthrosis Stress fracture Fibrous dysplasia Monostotic Polyostotic Skeletal fluorosis bone cyst Aneurysmal bone cyst Hyperostosis Infantile cortical hyperostosis Osteosclerosis Melorheostosis Pycnodysostosis Joint Chondritis Relapsing polychondritis Other Tietze's syndrome Combined Osteochondritis Osteochondritis dissecans Child leg: hip Legg–Calvé–Perthes syndrome tibia Osgood–Schlatter disease Blount's disease foot Köhler disease Sever's disease spine Scheuermann's_disease arm: wrist Kienböck's disease elbow Panner disease
-
Other Specified Feeding Or Eating Disorder
Wikipedia
Other specified feeding or eating disorder (OSFED) Specialty Psychiatry Other specified feeding or eating disorder ( OSFED ) is a DSM-5 category that, along with unspecified feeding or eating disorder (UFED), replaces the category formerly called eating disorder not otherwise specified ( EDNOS ) in the DSM-IV-TR . [1] It captures feeding disorders and eating disorders of clinical severity that do not meet diagnostic criteria for anorexia nervosa (AN), bulimia nervosa (BN), binge eating disorder (BED), avoidant/restrictive food intake disorder (ARFID), pica , or rumination disorder . [2] OSFED includes five examples: atypical anorexia nervosa, atypical bulimia nervosa of low frequency and/or limited duration, binge eating disorder of low frequency and/or limited duration, purging disorder , and night eating syndrome (NES). [2] Contents 1 Classification 2 Treatment 3 Epidemiology 4 History 5 References 6 External links Classification [ edit ] The five OSFED examples that can be considered eating disorders include atypical AN, BN (of low frequency and/or limited duration), BED (of low frequency and/or limited duration), purging disorder, and NES. ... Another term, Unspecified Feeding or Eating Disorder (UFED), is used to describe individuals for whom full diagnostic criteria are not met but the reason remains unspecified or the clinician does not have adequate information to make a more definitive diagnosis. [2] Atypical anorexia nervosa In atypical AN, individuals meet all of the criteria for AN, with the exception of the weight criterion: the individual's weight remains within or above the normal range, despite significant weight loss. [2] Atypical bulimia nervosa In this sub-threshold version of BN, individuals meet all criteria for BN, with the exception of the frequency criterion: binge eating and inappropriate compensatory behaviors occur, on average, less than once a week and/or for fewer than 3 months. [2] Binge-eating disorder of low frequency and/or limited duration In this sub-threshold version of BED, individuals must meet all criteria for BED, with the exception of the frequency criterion: binge eating occurs, on average, less than once a week and/or for fewer than 3 months. [2] Purging disorder In purging disorder, purging behavior aimed to influence weight or shape is present, but in the absence of binge eating. [2] Night eating syndrome In NES, individuals have recurrent episodes of eating at night, such as eating after awakening from sleep or excess calorie intake after the evening meal. ... "The Night Eating Questionnaire (NEQ): Psychometric properties of a measure of severity of the night eating syndrome". Eating Behaviors , 9 (1), 62-72. ^ a b c Fairburn C.G. , Cooper Z., Shafran R. (2003). ... Journal of Abnormal Psychology , 122 (2), 445-57. ^ Milano W, De Rosa M, Milano L, Capasso A (2012). "Night eating syndrome: an overview". Journal of Pharmacy and Pharmacology , 64 (1), 2-10. ^ Ornstein RM, Rosen DS, Mammel KA, Callahan ST, Forman S, Jay MS, Fisher M, Rome E, Walsh BT (2013).
-
Malignant Pleural Effusion
Wikipedia
External links [ edit ] Classification D ICD - 10-CM : J91.0 ICD - 9-CM : 511.81 MeSH : D016066 v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosisVEGFA, CEACAM5, EGFR, IL2, KRAS, ADA, ALK, ROMO1, CD274, CXCL8, IL17A, FGF2, IL1B, IL6, MUC1, KRT19, ROS1, CCL22, CXCL12, IL17D, IL27, ENO2, H3P10, CDKN2A, ACE, TMEM97, ATRNL1, WIF1, FSTL1, ESM1, CCL27, SEPTIN9, POSTN, WFDC2, DLEU1, CD163, EBAG9, BAP1, CCDC6, AREG, TNF, TLR2, TK1, NKX2-1, TIMP2, TERT, PDLIM3, EML4, SLPI, IL33, MIR4772, LINC01672, MIR93, MIR24-1, MIR21, MIR198, NUTM1, ALPP, APC, COL18A1, APOE, ASRGL1, MAP9, KIDINS220, MYDGF, NAT10, KRT20, XIAP, TLR8, FOXP3, ST2, SLC2A1, ERBB2, IFNG, KDR, ISG20, CDH1, IL15, IL10, CEACAM3, IL2RA, CEACAM7, CHI3L1, IFNA13, MS4A1, IFNA1, HSP90AB1, HP, HMGB1, FOLH1, CSF2, PTK2B, ETV4, ESR1, KIF5B, CD5, SHOX2, PTHLH, ATHS, CXCL11, BCL2, CCL11, CCL2, BRAF, RET, RAC1, PTPRC, CAPN1, LCN2, PLAU, NPC1, MYC, MUC5AC, MUC2, CD247, MMP9, MMP1, MDK, PSG2
-
Dens Evaginatus
Wikipedia
Premolars are more likely to be affected than any other tooth. [3] It could occur unilaterally or bilaterally. [1] Dens evaginatus (DE) typically occurs bilaterally and symmetrically. [4] This may be seen more frequently in Asians [3] (including Chinese , Malay , Thai , Japanese , Filipino and Indian populations). [4] The prevalence of DE ranges from 0.06% to 7.7% depending on the race. [3] It is more common in men than in women, [3] more frequent in the mandibular teeth than the maxillary teeth . [1] Patients with Ellis-van Creveld syndrome , incontinentia pigmenti achromians , Mohr syndrome , Rubinstein-Taybi syndrome and Sturge Weber syndrome are at a higher risk of having DE. [3] [2] Contents 1 Signs and symptoms 1.1 Associated anomalies 2 Cause 3 Diagnosis 3.1 Classification 4 Management 5 References 6 External links Signs and symptoms [ edit ] It is important to diagnose DE early and provide appropriate treatment to help prevent periodontal disease , caries , pulpal complications [3] and malocclusion . [2] It occurs on the cingulum /occlusal surface of the teeth.
-
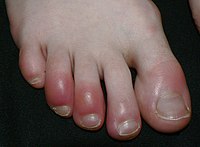
Chilblains
Wikipedia
In infants affected by Aicardi–Goutières syndrome (a rare inherited condition which affects the nervous system ) chilblain-like symptoms occur together with severe neurologic disturbances and unexplained fevers. ... DermAtlas 1683395337 Cold stress , National Institute for Occupational Safety and Health Classification D ICD - 10 : T69.1 ICD - 9-CM : 991.5 MeSH : D002647 DiseasesDB : 31219 External resources eMedicine : derm/322 v t e Consequences of external causes Temperature Elevated Hyperthermia Heat syncope Reduced Hypothermia Immersion foot syndromes Trench foot Tropical immersion foot Warm water immersion foot Chilblains Frostbite Aerosol burn Cold intolerance Acrocyanosis Erythrocyanosis crurum Radiation Radiation poisoning Radiation burn Chronic radiation keratosis Eosinophilic, polymorphic, and pruritic eruption associated with radiotherapy Radiation acne Radiation-induced cancer Radiation recall reaction Radiation-induced erythema multiforme Radiation-induced hypertrophic scar Radiation-induced keloid Radiation-induced morphea Air Hypoxia / Asphyxia Barotrauma Aerosinusitis Decompression sickness High altitude Altitude sickness Chronic mountain sickness Death zone HAPE HACE Food Starvation Maltreatment Physical abuse Sexual abuse Psychological abuse Travel Motion sickness Seasickness Airsickness Space adaptation syndrome Adverse effect Hypersensitivity Anaphylaxis Angioedema Allergy Arthus reaction Adverse drug reaction Other Electrical injury Drowning Lightning injuries Ungrouped skin conditions resulting from physical factors Dermatosis neglecta Pinch mark Pseudoverrucous papules and nodules Sclerosing lymphangitis Tropical anhidrotic asthenia UV-sensitive syndrome environmental skin conditions Electrical burn frictional/traumatic/sports Black heel and palm Equestrian perniosis Jogger's nipple Pulling boat hands Runner's rump Surfer's knots Tennis toe Vibration white finger Weathering nodule of ear Wrestler's ear Coral cut Painful fat herniation Uranium dermatosis iv use Skin pop scar Skin track Slap mark Pseudoacanthosis nigricans Narcotic dermopathy Authority control NDL : 00573416
-
Periodontitis, Aggressive, 1
OMIM
This interval overlapped the region of chromosome 11q14 containing the CTSC gene (602365), mutations in which can cause Papillon-Lefevre (245000) and Haim-Munk (245010) syndromes. Genetic Heterogeneity Roulston et al. (1985) studied dentinogenesis imperfecta (DGI; 125490) in the triracial population of Brandywine, Maryland, and found that a localized form of juvenile periodontitis (JP) was cosegregating. ... They suggested that the disorder is genetically heterogeneous and that one form represents a partially penetrant Papillon-Lefevre syndrome. Association Studies Amer et al. (1988) reported evidence for an association between HLA alleles and susceptibility to periodontitis. ... INHERITANCE - Autosomal recessive HEAD & NECK Mouth - Severe, early-onset periodontitis - Alveolar bone destruction - Gingival recession Teeth - Premature tooth loss SKIN, NAILS, & HAIR Skin - No palmoplantar keratosis MISCELLANEOUS - Genetic heterogeneity - Allelic to Papillon-Lefevre syndrome ( 245000 ) and Haim-Munk syndrome ( 245010 ) MOLECULAR BASIS - Caused by mutation in the cathepsin C gene (CTSC, 602365.0012 ) ▲ CloseCTSC, POSTN, SIGLEC5, IL10, IL1A, TNF, IL1B, OSTCP2, IL6, TLR4, IL4, FPR1, IL13, CXCL8, GLT6D1, VDR, CD14, IL1RN, IFNG, DEFB1, ITGB2, IL36RN, CCL2, HLA-DRB1, HLA-DQB1, IL37, S100A8, CTLA4, BRINP3, CDKN2B-AS1, CAMP, MMP8, NOS2, IL17C, WNT5A, HLA-DQA1, CCR5, IL23A, CSF1, STAT1, RBM45, FCGR3B, FCGR3A, TNFRSF11B, NOD2, PLG, ITGAM, IGF1R, HSPB3, ADAM23, IL1R2, CNOT8, ZNF136, DEFA1A3, DEFA1B, VCAM1, SFXN1, TYK2, TPO, TP53, TNFRSF1B, AIM2, CCR2, TLR2, TIMP2, TRBV20OR9-2, SLC6A4, SELE, CCL3, DEFB4B, SCN4A, TGFBRAP1, PES1, CIR1, AP1S3, GPRIN1, UBE3D, MMP28, MMP25, POPDC2, EEFSEC, SLAMF7, BEGAIN, ADGRG6, SELENOS, SMPD3, TREM1, HSPA14, IL20, KRT25, SLC23A1, IL19, PTGS2, CKAP2L, PYDC2, GPRC6A, KRT23, IL17RA, IFNL2, IFNL3, IFNL1, UCN2, H19, IL24, NOD1, ALOX5, MPO, PRTN3, FCGR2A, DECR1, DEFA1, DEFB4A, ATN1, ELN, ESR2, FCAR, GATA3, HSPB1, GC, GNAS, CXCR3, GSTM1, GSTT1, HLA-A, HLA-B, DGKA, CYP1A1, CYBA, CTSD, BAD, CFB, PRDM1, BTF3P11, CASP8, CASP9, CD28, CDB2, CDKN2A, CDKN2B, CDX2, CLU, CCR6, KLF6, CSF3, HLA-C, HSPB2, HTRA1, COX2, CXCL9, MKLN1, MMP1, MMP2, MMP3, MMP9, APOH, MUC2, HSPD1, MUC5AC, MUC6, NOTCH1, PAFAH1B1, SERPINA1, PI3, PON1, MBL2, SMAD7, SMAD4, LTF, IL1R1, IL2, IL2RA, IL12RB2, IL17A, IL18, INHA, CXCL10, IRF5, ISG20, ITGAL, KCNJ5, LCN2, LRPAP1, LTA, MTCO2P12
-
Obstructive Lung Disease
Wikipedia
External links [ edit ] Classification D MeSH : D008173 v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosisCCNO, NR3C1, FOXF1, DNAAF1, PIH1D3, DNAL1, CCDC151, LRRC56, RPGR, CCDC114, DRC1, RSPH1, SPAG1, CCDC65, OFD1, DNAH11, CFAP300, LRRC6, DNAH1, DNAI1, STK36, NME8, ZMYND10, HYDIN, DNAAF5, CCDC40, ARMC4, DNAAF2, CFAP298, DNAI2, RSPH3, MGP, TTC25, CCDC103, COPD, APC, DNAAF4, GLA, DNASE1L3, DNAH5, CCDC39, RSPH4A, GAS8, GAS2L2, DNAAF3, DNAJB13, RSPH9, MCIDAS, SERPINA1, CFTR, SERPINA3, GCG, TNF, GLP1R, SCNN1B, CRP, IL1A, IL1B, ADRB2, POTEM, SFTPA1, MUC5B, POTEKP, DNAH14, MIR106B, MAGT1, ACTBL2, TSLP, BMF, SLC26A9, A2M, FHL5, SLC2A10, FEV, ACTG1, ACTG2, ALPI, ALPP, CAT, CD47, CHRNA3, COL4A5, CX3CR1, ELN, FLNA, CXCR3, HDAC2, IAPP, IL17A, LCN1, LTC4S, MBL2, MMP1, MUC5AC, P2RX3, PDE4A, CX3CL1, SFTPB, SFTPC, SFTPD, SCGB1A1, GPR68, ACOT7, SFTPA2
-
Myasthenia Gravis
OMIM
Several mothers with clinically diagnosed myasthenia gravis have given birth to infants with the Pena-Shokeir syndrome (208150), which is characterized by pulmonary hypoplasia, multiple ankyloses, and facial abnormalities. ... In the case of maternal myasthenia gravis, the recurrence risk for Pena-Shokeir syndrome is high, and there has been no instance of a normal child being born following the affected pregnancy. ... Among the 7 children with congenital myasthenic syndromes, severity varied. The diagnosis in severe cases was often obscured by apnea attacks, aspiration, and failure to thrive. ... Croxen et al. (2002) reported 2 sisters diagnosed in childhood with congenital myasthenic syndrome, each of whom was found to carry 2 mutations in the AChR epsilon-subunit gene, near the N terminus.CFB, HLA-B, MUSK, HLA-DPB1, POMC, FAS, HLA-DRB1, HLA-DQA1, PTPN22, HLA-A, TNIP1, C2, IL10, NFKBIL1, ZNRD1, MUC21, SFTA2, HCG9, PSORS1C1, CTLA4, NOTCH4, MUCL3, CYP21A2, RBM45, BTNL2, GPSM3, MSH5, TSBP1, MICB, LRP4, TRIM31, POU5F1, HLA-DQA2, RNF39, GABBR1, VARS2, LINC00243, ABCF1, IFNG, MSH5-SAPCD1, HCG17, TNFRSF11A, TCF19, BCHE, ATP6V1G2, STK19, TNF, HCG18, GPANK1, SEMA5A, TTN, TSBP1-AS1, RBBP8, ACHE, PRRC2A, CXCL13, IL17A, IL2RA, IL6, ISG20, EIF3K, IL2, FOXP3, AIRE, IL4, CHRNA1, TRBV20OR9-2, HLA-DQB1, THM, LTA, IL1B, CD274, IL22, PDCD1, IL21, TLR9, CHRNE, IL1A, MIR150, AQP4, HT, TGFB1, CDR3, ECD, MIR21, DOK7, TLR4, CD40, TLR3, MBP, CCL21, CHRNA4, TAP2, CXCR4, IGHG3, IFNB1, MAPK1, PDLIM7, IL18R1, IL15, EBI3, IL4R, SMN1, CXCL10, IFNA13, TLR7, TNFRSF13C, FGFR3, MIR146A, ESR1, TSLP, CD40LG, GNAO1, DNMT3B, HLA-DQB2, CAV3, IL23A, MIR125A, ADRB2, IFNA1, IFN1@, HMGB1, C4orf3, DIPK1A, SOCS3, LGI1, MSC, SCO2, CD83, GRAP2, MIR145, MIRLET7C, NTN1, MIR155, PPP6R2, MIR143, MBTPS1, MIR15B, SCFV, LOC102723407, IFNG-AS1, LINC-ROR, C4B_2, C20orf181, TEC, CCR2, DDX39B, MIR653, MIR323B, MIR19B1, MIR338, AIMP2, FOSL1, MIR320A, USO1, TNFRSF25, MIR30E, MALAT1, TNFSF10, DDX39A, RMDN2, MYAS1, CCAR2, RNF19A, CNTNAP2, HIF3A, ROBO3, POLDIP2, IFIH1, IGAN1, B3GAT1, DPYSL5, PART1, RETN, IGHV3-52, TWNK, MSL2, KRT20, ICOS, SLC25A37, VAV1, TMEM109, PPP1R15A, PRSS16, UNC5A, CLEC4C, CDIPT, NXF1, MZB1, TRIM9, AHSA1, IL17F, IL33, TNFSF13B, DDX58, CCR9, FHDC1, LILRB1, FAM136A, SLC7A9, TBC1D9, ICOSLG, SEC14L2, VIP, RAF1, UTRN, CNTFR, CRK, MAPK14, CSF1, CCN2, CTSV, CTSS, CYP3A5, CD55, BRINP1, DCC, DNMT3A, ATN1, TYMP, CTTN, ERBB4, ESR2, FCGR2A, FLNB, FOS, FOSB, CXCR3, GRIA2, GRM2, CXCL1, GZMB, HLA-C, HLA-DOA, HLA-DPA1, HLA-DRB3, CR2, CCR7, HNMT, CCR5, ADCYAP1, AGER, ALB, APOE, APRT, ABCC6, BCL2, TNFRSF17, BDNF, C4A, C4B, C5, CA3, CACNA1S, CALCA, CALCR, CAMP, CASP1, CASP3, CD19, MS4A1, CD28, CD86, CD69, CDS1, CHRNB1, CHRND, CLC, CCR4, HLA-G, HOXD13, TYMS, NTRK1, P2RX7, PAM, PAX7, ABCB1, PMP22, MAPK3, PTPRC, PLAAT4, RELB, S100A8, S100A11, S100B, SCN4A, SCO1, CCL5, CCL17, CCL22, CXCL12, SGCA, SLAMF1, SMN2, SPP1, STAT3, STAT4, TAP1, THBS1, TNFAIP3, TNFSF4, TNFRSF4, OSM, NCAM1, HSPA5, MYOG, IRF8, IFNA2, IFNA17, IFNGR1, IGF1, IGF1R, IGFBP1, IGL, IL1RN, IL2RB, IL7R, IL9, IL12B, IL12RB2, INS, IRF4, ITGAX, JUN, JUNB, JUND, KIT, KRT5, LDLR, LGALS1, LGALS8, LIF, MEFV, MFAP1, MMP10, LOC102724971
-
Lama2 Muscular Dystrophy
GeneReviews
Affected individuals may show muscle hypertrophy and develop a rigid spine syndrome with joint contractures, usually most prominent in the elbows. ... Sparing of the gracilis, sartorius, vastus medialis, and rectus femoris muscles has also been described [Nelson et al 2015]. Individuals with rigid spine syndrome had sparing of temporal muscles, except in those associated with biallelic LAMA2 pathogenic variants [Tordjman et al 2018]. ... Affected individuals may show muscle hypertrophy and develop a rigid spine syndrome with joint contractures, usually most prominent in the elbows. ... Some individuals have rigid spine syndrome and/or muscle pseudohypertrophy [Nelson et al 2015]. ... The disorders included in the differential diagnosis are other congenital muscular dystrophies, congenital myopathies, congenital myasthenic syndromes, and spinal muscular atrophy.
-
Genetic Atypical Hemolytic-Uremic Syndrome
GeneReviews
Summary Clinical characteristics. Hemolytic-uremic syndrome (HUS) is characterized by hemolytic anemia, thrombocytopenia, and renal failure caused by platelet thrombi in the microcirculation of the kidney and other organs. ... Diagnosis Suggestive Findings Genetic atypical hemolytic-uremic syndrome (aHUS) should be suspected in a proband with a diagnosis of aHUS in addition to ONE of the following criteria: Two or more members of the same family have been diagnosed with aHUS at least six months apart and exposure to a common triggering infectious agent has been excluded. ... Clinical Characteristics Clinical Description The onset of atypical hemolytic-uremic syndrome (aHUS) ranges from the neonatal period to adulthood. ... Some women progress to a life-threatening variant of preeclampsia with severe thrombocytopenia, microangiopathic hemolytic anemia, renal failure, and liver involvement (HELLP syndrome). Complete remission usually follows prompt delivery. ... Underlying medical conditions include autoimmune disease (e.g., scleroderma, anti-phospholipid syndrome, systemic lupus erythematosus).
-
Premature Ejaculation
Wikipedia
John Mulhall], when we talk casually about premature ejaculation ... we're usually talking about what the medical community would consider 'premature-ejaculatory-like syndrome,' or simply 'rapid ejaculation.' ... ... External links [ edit ] Classification D ICD - 10 : F52.4 ICD - 9-CM : 302.75 MeSH : D061686 External resources MedlinePlus : 001524 eMedicine : med/643 Patient UK : Premature ejaculation v t e Outline of human sexuality Physiology and biology Erection Insemination Intersex Libido Nocturnal emission Orgasm Female and male ejaculation Pelvic thrust Pre-ejaculate Pregnancy Sexual arousal Sexual stimulation Health and education Birth control Condom Masters and Johnson Reproductive medicine Andrology Gynaecology Urology Safe sex Sex education Sex therapy ( PLISSIT model ) Sexology Sexual dysfunction Erectile dysfunction Hypersexuality Hyposexuality Sexual medicine Sexual surrogate Sexually transmitted infection Identity and diversity Gender binary Gender identity Men who have sex with men Sexual identity Sexual orientation Women who have sex with women Law Age of consent Criminal transmission of HIV Child sexual abuse Incest Indecent exposure Obscenity Sexual abuse Cybersex trafficking Rape Sex trafficking Sexual assault Sexual harassment Sexual misconduct Sexual slavery Sexual violence History Blue Movie Counterculture of the 1960s Feminist sex wars Golden Age of Porn History of erotic depictions Sexual revolution Relationships and society Anarchism and love/sex Extramarital sex Family planning Flirting Free love Marriage Modesty Polyamory Premarital sex Promiscuity Romance Sex-positive movement Sexual abstinence Sexual addiction Sexual attraction Sexual capital Sexual ethics Sexual objectification Sexual slang By country Ancient Rome China India Japan Philippines South Korea United States Sexual activities Conventional sex Anal sex Bareback BDSM Child sex Creampie Edging Erotic sexual denial Fetishism Fingering Fisting Gang bang Group sex Masturbation Mechanics of sex Nipple stimulation Non-penetrative sex Facial Foot fetishism Footjob Forced orgasm Frot Handjob Mammary intercourse Sumata Oral sex 69 Anilingus Cunnilingus Fellatio Irrumatio Paraphilia Pompoir Quickie Sex in space Sex positions Sexual fantasy Sexual fetishism Sexual intercourse Foreplay Sexual penetration Swinging Tribadism Urethral intercourse Urolagnia Virtual sex Cybersex Erotic talk Wet T-shirt contest Sex industry Red-light district Adult video games Erotica Pornography Film actor Prostitution Survival sex Sex museum Sex shop Sex tourism Child Female Sex worker Sex toy doll Strip club Webcam model Religion and sexuality Buddhism Christian demonology Daoism Islam Mormonism Sex magic Human sexuality portal v t e Mental and behavioral disorders Adult personality and behavior Gender dysphoria Ego-dystonic sexual orientation Paraphilia Fetishism Voyeurism Sexual maturation disorder Sexual relationship disorder Other Factitious disorder Munchausen syndrome Intermittent explosive disorder Dermatillomania Kleptomania Pyromania Trichotillomania Personality disorder Childhood and learning Emotional and behavioral ADHD Conduct disorder ODD Emotional and behavioral disorders Separation anxiety disorder Movement disorders Stereotypic Social functioning DAD RAD Selective mutism Speech Stuttering Cluttering Tic disorder Tourette syndrome Intellectual disability X-linked intellectual disability Lujan–Fryns syndrome Psychological development ( developmental disabilities ) Pervasive Specific Mood (affective) Bipolar Bipolar I Bipolar II Bipolar NOS Cyclothymia Depression Atypical depression Dysthymia Major depressive disorder Melancholic depression Seasonal affective disorder Mania Neurological and symptomatic Autism spectrum Autism Asperger syndrome High-functioning autism PDD-NOS Savant syndrome Dementia AIDS dementia complex Alzheimer's disease Creutzfeldt–Jakob disease Frontotemporal dementia Huntington's disease Mild cognitive impairment Parkinson's disease Pick's disease Sundowning Vascular dementia Wandering Other Delirium Organic brain syndrome Post-concussion syndrome Neurotic , stress -related and somatoform Adjustment Adjustment disorder with depressed mood Anxiety Phobia Agoraphobia Social anxiety Social phobia Anthropophobia Specific social phobia Specific phobia Claustrophobia Other Generalized anxiety disorder OCD Panic attack Panic disorder Stress Acute stress reaction PTSD Dissociative Depersonalization disorder Dissociative identity disorder Fugue state Psychogenic amnesia Somatic symptom Body dysmorphic disorder Conversion disorder Ganser syndrome Globus pharyngis Psychogenic non-epileptic seizures False pregnancy Hypochondriasis Mass psychogenic illness Nosophobia Psychogenic pain Somatization disorder Physiological and physical behavior Eating Anorexia nervosa Bulimia nervosa Rumination syndrome Other specified feeding or eating disorder Nonorganic sleep Hypersomnia Insomnia Parasomnia Night terror Nightmare REM sleep behavior disorder Postnatal Postpartum depression Postpartum psychosis Sexual dysfunction Arousal Erectile dysfunction Female sexual arousal disorder Desire Hypersexuality Hypoactive sexual desire disorder Orgasm Anorgasmia Delayed ejaculation Premature ejaculation Sexual anhedonia Pain Nonorganic dyspareunia Nonorganic vaginismus Psychoactive substances, substance abuse and substance-related Drug overdose Intoxication Physical dependence Rebound effect Stimulant psychosis Substance dependence Withdrawal Schizophrenia , schizotypal and delusional Delusional Delusional disorder Folie à deux Psychosis and schizophrenia-like Brief reactive psychosis Schizoaffective disorder Schizophreniform disorder Schizophrenia Childhood schizophrenia Disorganized (hebephrenic) schizophrenia Paranoid schizophrenia Pseudoneurotic schizophrenia Simple-type schizophrenia Other Catatonia Symptoms and uncategorized Impulse control disorder Klüver–Bucy syndrome Psychomotor agitation Stereotypy
-
Breech Birth
Wikipedia
Endogenous factors involve fetal inability to adequately move, whereas exogenous factors refer to insufficient intrauterine space available for fetal movements. [15] Incidence of breech presentation among diseases and medical conditions with the incidence of breech presentation higher than occurs in the general population, shows that the probability of breech presentation is between 4% and 50%. [16] [17] [18] These data are related to: single series of medical entities collections of series for some particular medical entity data obtained from repeated observations under the same conditions series of two concomitant medical conditions Rates in various medical conditions [ edit ] Fetal entities: First twin 17–30%; Second twin 28–39%; Stillborn 26%; Prader–Willi syndrome 50%, Werdnig–Hoffman syndrome 10%; Smith–Lemli–Opitz syndrome 40%; Fetal alcohol syndrome 40%; Potter anomaly 36%; Zellweger syndrome 27%; Myotonic dystrophy 21%, 13 trisomy syndrome 12%; 18 trisomy syndrome 43%; 21 trisomy syndrome 5%; de Lange syndrome 10%; Anencephalus 6–18%, Spina bifida 20–30%; Congenital hydrocephalus 24–37%; Osteogenesis imperfecta 33.3%; Amyoplasia 33.3%; Achondrogenesis 33.3%; Amelia 50%; Craniosynostosis 8%; Sacral agenesis 30.4%; Arthrogriposis multiplex congenita 33.3; Congenital dislocation of the hip 33.3%; Hereditary sensory neuropathy type III 25%; Centronuclear myopathy 16.7%; Multiple pituitary hormone deficiency 50%; Isolated pituitary hormone deficiency 20%; Ectopic posterior pituitary gland 33.3%; Congenital bilateral perisilvian syndrome 33.3; Symmetric fetal growth restriction 40%; Asymmetric fetal growth restriction 40%; Nonimmune hydrops fetalis 15%; Atresia ani 18.2%; Microcephalus 15.4%; Omphalocele 12.5%; Prematurity 40% Placental and amniotic fluid entities: Amniotic sheet perpendicular to the placenta 50%; cornual–fundal implantation of the placenta 30%; Placenta previa 12.5%; Oligohydramnios 17%; Polyhydramnios 15.8% Maternal entities: Uterus arcuatus 22.6%; Uterus unicornuatus 33.3%; Uterus bicornuatus 34.8%; Uterus didelphys 30–41%; Uterus septus 45.8%; Leiomyoma uteri 9–20%; Spinal cord injury 10%; Carriers of Duchenne muscular dystrophy 17% Combination of two medical entities: First twin in uterus with two bodies 14.29%; Second twin in uterus with two bodies 18.52%. [18] Also, women with previous Caesarean deliveries have a risk of breech presentation at term twice that of women with previous vaginal deliveries. [19] The highest possible probability of breech presentation of 50% indicates that breech presentation is a consequence of random filling of the intrauterine space, with the same probability of breech and cephalic presentation in a longitudinally elongated uterus. [17] Types [ edit ] Types of breech depend on how the baby's legs are lying. [14] A frank breech (otherwise known as an extended breech) is where the baby's legs are up next to its abdomen, with its knees straight and its feet next to its ears. ... External links [ edit ] Classification D ICD - 10 : O32.1 , O64.1 , O80.1 , O83.0 , P03.0 ICD - 9-CM : 652.1 MeSH : D001946 DiseasesDB : 1631 External resources MedlinePlus : 002060 eMedicine : med/3272 emerg/868 Breech birth controversies in Great Britain GLOWM video demonstrating vaginal breech delivery techniques v t e Pathology of pregnancy , childbirth and the puerperium Pregnancy Pregnancy with abortive outcome Abortion Ectopic pregnancy Abdominal Cervical Interstitial Ovarian Heterotopic Embryo loss Fetal resorption Molar pregnancy Miscarriage Stillbirth Oedema , proteinuria and hypertensive disorders Gestational hypertension Pre-eclampsia HELLP syndrome Eclampsia Other, predominantly related to pregnancy Digestive system Acute fatty liver of pregnancy Gestational diabetes Hepatitis E Hyperemesis gravidarum Intrahepatic cholestasis of pregnancy Integumentary system / dermatoses of pregnancy Gestational pemphigoid Impetigo herpetiformis Intrahepatic cholestasis of pregnancy Linea nigra Prurigo gestationis Pruritic folliculitis of pregnancy Pruritic urticarial papules and plaques of pregnancy (PUPPP) Striae gravidarum Nervous system Chorea gravidarum Blood Gestational thrombocytopenia Pregnancy-induced hypercoagulability Maternal care related to the fetus and amniotic cavity amniotic fluid Oligohydramnios Polyhydramnios Braxton Hicks contractions chorion / amnion Amniotic band syndrome Chorioamnionitis Chorionic hematoma Monoamniotic twins Premature rupture of membranes Obstetrical bleeding Antepartum placenta Circumvallate placenta Monochorionic twins Placenta accreta Placenta praevia Placental abruption Twin-to-twin transfusion syndrome Labor Amniotic fluid embolism Cephalopelvic disproportion Dystocia Shoulder dystocia Fetal distress Locked twins Nuchal cord Obstetrical bleeding Postpartum Pain management during childbirth placenta Placenta accreta Preterm birth Postmature birth Umbilical cord prolapse Uterine inversion Uterine rupture Vasa praevia Puerperal Breastfeeding difficulties Low milk supply Cracked nipples Breast engorgement Childbirth-related posttraumatic stress disorder Diastasis symphysis pubis Postpartum bleeding Peripartum cardiomyopathy Postpartum depression Postpartum psychosis Postpartum thyroiditis Puerperal fever Puerperal mastitis Other Concomitant conditions Diabetes mellitus Systemic lupus erythematosus Thyroid disorders Maternal death Sexual activity during pregnancy Category v t e Pregnancy and childbirth Planning Birth control Natural family planning Pre-conception counseling Conception Assisted reproductive technology Artificial insemination Fertility medication In vitro fertilisation Fertility awareness Unintended pregnancy Testing 3D ultrasound Obstetric ultrasonography Pregnancy test Home testing Prenatal diagnosis Prenatal Anatomy Amniotic fluid Amniotic sac Endometrium Placenta Development Fundal height Gestational age Human embryogenesis Maternal physiological changes Postpartum physiological changes Care Nutrition Environmental toxicants In pregnancy Prenatal Concomitant conditions Drinking Diabetes mellitus Smoking Vaping SLE Sexual activity during pregnancy Procedures Amniocentesis Cardiotocography Chorionic villus sampling Nonstress test Abortion Childbirth Preparation Bradley method Hypnobirthing Lamaze Nesting instinct Roles Doula Birth attendant Men's roles Midwife Obstetrician Perinatal nurse Traditional birth attendant Delivery Bloody show Childbirth positions Home birth Multiple birth Natural childbirth Pelvimetry / Bishop score Cervical dilation Cervical effacement Position Presentation Breech Cephalic Shoulder Rupture of membranes Unassisted childbirth Uterine contraction Water birth Postpartum Maternal Postpartum confinement Sex after pregnancy Psychiatric disorders of childbirth Postpartum physiological changes Roles Doula Health visitor Lactation consultant Monthly nurse Confinement nanny Infant Adaptation to extrauterine life Child care Congenital disorders Obstetric history Gravidity and parity
-
Inflammatory Demyelinating Diseases Of The Central Nervous System
Wikipedia
These conditions can appear as Neuromyelitis optica (NMO), and its associated "spectrum of disorders" (NMOSD), currently considered a common syndrome for several separated diseases [20] but with some still idiopathic subtypes. ... This is often named "Radiologically Isolated Syndrome" (RIS). Cases before the first attack or CIS are subclinical in the sense that they do not produce clinical situations. ... "Pattern Recognition of the Multiple Sclerosis Syndrome" . Brain Sciences . 7 (10): 138. doi : 10.3390/brainsci7100138 . ... S2CID 22270592 . ^ Wingerchuk, Dean (2006). "Neuromyelitis Optica (Devic's Syndrome)" (PDF) . 2006 Rare Neuroimmunologic Disorders Symposium . ... "Atypical inflammatory demyelinating syndromes of the CNS". The Lancet Neurology . 15 (9): 967–981. doi : 10.1016/S1474-4422(16)30043-6 .
-
Premature Ventricular Contraction
Wikipedia
. ^ Lebowitz, Michael. "Methylxanthine Toxcity Syndrome" . Body Restoration: An Owner's Manual . ... External links [ edit ] Classification D ICD - 10 : I49.3 ICD - 9-CM : 427.69 MeSH : D018879 DiseasesDB : 32412 External resources eMedicine : emerg/773 v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic feverNOS3, SCN5A, TMEM43, LMNA, DSG2, TTN-AS1, DSP, MYBPC3, TTN, JUP, NAA10, RYR1, FAF1, TRDN, TNNI3K, CACNA1S, SLC25A20, RYR2, CASQ2, SLC6A8, KCNH2, HHIP, ST13, SULT1E1, PAGR1, KCNE5, LRIG1, FGF23, PACC1, TRPM4, LRIG2, KCNE2, UGCG, ATP5F1A, RPL29, PTH, CALCR, CALM3, CALR, CD59, CRP, ACE, DNM2, ELANE, EMD, FLNC, GAST, GALNS, GCLC, KCNJ2, KCNQ1, LRP5, BCL2A1, REG3A, PLN, ORM1
-
Thiamine Deficiency
Wikipedia
It is characterized by: Difficulty in walking Tingling or loss of sensation ( numbness ) in hands and feet Loss of tendon reflexes [10] Loss of muscle function or paralysis of the lower legs Mental confusion/speech difficulties Pain Involuntary eye movements ( nystagmus ) Vomiting A selective impairment of the large proprioceptive sensory fibers without motor impairment can occur and present as a prominent sensory ataxia , which is a loss of balance and coordination due to loss of the proprioceptive inputs from the periphery and loss of position sense. [11] Brain disease [ edit ] Wernicke's encephalopathy (WE), Korsakoff syndrome (alcohol amnestic disorder), and Wernicke–Korsakoff syndrome are forms of dry beriberi. [4] Wernicke's encephalopathy is the most frequently encountered manifestation of thiamine deficiency in Western society, [12] [13] though it may also occur in patients with impaired nutrition from other causes, such as gastrointestinal disease, [12] those with HIV/AIDS , and with the injudicious administration of parenteral glucose or hyperalimentation without adequate B-vitamin supplementation. [14] This is a striking neuro-psychiatric disorder characterized by paralysis of eye movements, abnormal stance and gait, and markedly deranged mental function. [15] Korsakoff syndrome is, in general, considered to occur with deterioration of brain function in patients initially diagnosed with WE. [16] This is an amnestic-confabulatory syndrome characterized by retrograde and anterograde amnesia , impairment of conceptual functions, and decreased spontaneity and initiative. [17] Alcoholics may have thiamine deficiency because of the following: Inadequate nutritional intake: Alcoholics tend to intake less than the recommended amount of thiamine. ... Other disorders in which a putative role for thiamine has been implicated include subacute necrotising encephalomyelopathy , opsoclonic cerebellopathy (a paraneoplastic syndrome), and Nigerian seasonal ataxia . ... "Gastrointestinal Beriberi: A Previously Unrecognized Syndrome". Ann Intern Med . 141 (11): 898–899. doi : 10.7326/0003-4819-141-11-200412070-00035 . ... Baltimore: Lippincott Williams & Wilkins; 1999 ^ Maurice V, Adams RD, Collins GH. The Wernicke-Korsakoff Syndrome and Related Neurologic Disorders Due to Alcoholism and Malnutrition . 2nd ed. ... "Wild birds of declining European species are dying from a thiamine deficiency syndrome" . Proc Natl Acad Sci U S A . 106 (29): 12001–12006.
-
Concussions In Sport
Wikipedia
Both immediate and delayed symptoms can continue for long periods of time and have a negative impact on recovery. [5] Post-concussion syndrome [ edit ] There is the potential of post-concussion syndrome , defined as a set of symptoms that may continue after a concussion is sustained. [6] Post-concussion symptoms can be classified into physical, cognitive, emotional, and sleep symptoms. [6] Physical symptoms include a headache, nausea, and vomiting. [6] Athletes may experience cognitive symptoms that include speaking slowly, difficulty remembering and concentrating. [6] Emotional and sleep symptoms include irritability, sadness, drowsiness, and trouble falling asleep. [6] Second-impact syndrome [ edit ] Ignoring concussions makes athletes more vulnerable to incurring further head trauma, stressing the importance of rigorous concussion testing protocols in professional sports . Subsequent impact can cause a rare condition known as second-impact syndrome , which can result in severe injury or death. [7] Second-impact syndrome can as a result of a second head injury before the brain has adequate time to heal in between concussions. [8] It typically give signs and symptoms of a post-concussion syndrome (visual, motor, or sensory abnormalities and difficulties with cognitive processes). ... For the consequences of concussion, the UK and Ireland mentioned “Second Impact Syndrome “(22.2%), “Chronic Traumatic Encephalopathy” (22.2%) and “Parkinson's disease and other neurological conditions” (11.1%) the most. ... International Journal of Athletic Therapy and Training . 16 (5): 5–9. doi : 10.1123/ijatt.16.5.5 . ^ a b c d e Ganti, Latha; Khalid, Hussain; Patel, Pratik Shashikant; Daneshvar, Yasamin; Bodhit, Aakash N; Peters, Keith R (2014). "Who gets post-concussion syndrome? An emergency department-based prospective analysis" . ... PMID 25635191 . ^ Bey, T; Ostick, B (2009). "Second impact syndrome" . The Western Journal of Emergency Medicine . 10 (1): 6–10.