Interstitial Cystitis
Overview
Interstitial cystitis (in-tur-STISH-ul sis-TIE-tis) is a chronic condition causing bladder pressure, bladder pain and sometimes pelvic pain. The pain ranges from mild discomfort to severe pain. The condition is a part of a spectrum of diseases known as painful bladder syndrome.
Your bladder is a hollow, muscular organ that stores urine. The bladder expands until it's full and then signals your brain that it's time to urinate, communicating through the pelvic nerves. This creates the urge to urinate for most people.

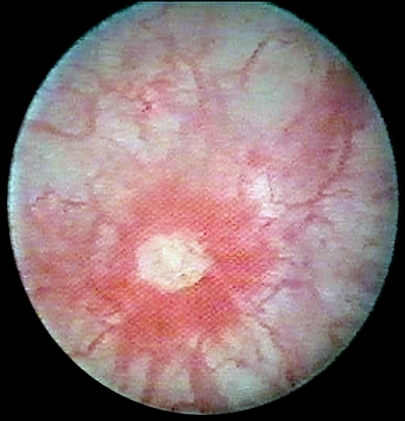
Interstitial cystitis
Your bladder, kidneys, ureters and urethra make up your urinary system. When you have interstitial cystitis, the walls of your bladder become irritated and inflamed (shown right), compared with those of a normal bladder (shown top).
With interstitial cystitis, these signals get mixed up — you feel the need to urinate more often and with smaller volumes of urine than most people.
Interstitial cystitis most often affects women and can have a long-lasting impact on quality of life. Although there's no cure, medications and other therapies may offer relief.
Symptoms
The signs and symptoms of interstitial cystitis vary from person to person. If you have interstitial cystitis, your symptoms may also vary over time, periodically flaring in response to common triggers, such as menstruation, sitting for a long time, stress, exercise and sexual activity.
Interstitial cystitis signs and symptoms include:
- Pain in your pelvis or between the vagina and anus in women
- Pain between the scrotum and anus (perineum) in men
- Chronic pelvic pain
- A persistent, urgent need to urinate
- Frequent urination, often of small amounts, throughout the day and night (up to 60 times a day)
- Pain or discomfort while the bladder fills and relief after urinating
- Pain during sex
Symptoms severity is different for everyone, and some people may experience symptom-free periods.
Although signs and symptoms of interstitial cystitis may resemble those of a chronic urinary tract infection, there's usually no infection. However, symptoms may worsen if a person with interstitial cystitis gets a urinary tract infection.
When to see a doctor
If you're experiencing chronic bladder pain or urinary urgency and frequency, contact your health care provider.
Causes
The exact cause of interstitial cystitis isn't known, but it's likely that many factors contribute. For instance, people with interstitial cystitis may also have a defect in the protective lining (epithelium) of the bladder. A leak in the epithelium may allow toxic substances in urine to irritate your bladder wall.
Other possible but unproven contributing factors include an autoimmune reaction, heredity, infection or allergy.
Risk factors
These factors are associated with a higher risk of interstitial cystitis:
- Your sex. Women are diagnosed with interstitial cystitis more often than men. Symptoms in men may mimic interstitial cystitis, but they're more often associated with an inflammation of the prostate gland (prostatitis).
- Your age. Most people with interstitial cystitis are diagnosed during their 30s or older.
- Having a chronic pain disorder. Interstitial cystitis may be associated with other chronic pain disorder, such as irritable bowel syndrome or fibromyalgia.
Complications
Interstitial cystitis can result in a number of complications, including:
- Reduced bladder capacity. Interstitial cystitis can cause stiffening of the bladder wall, which allows your bladder to hold less urine.
- Lower quality of life. Frequent urination and pain may interfere with social activities, work and other activities of daily life.
- Sexual intimacy problems. Frequent urination and pain may strain your personal relationships, and sexual intimacy may suffer.
- Emotional troubles. The chronic pain and interrupted sleep associated with interstitial cystitis may cause emotional stress and can lead to depression.
Diagnosis
Diagnosis of interstitial cystitis might include:
- Medical history and bladder diary. Your health care provider may ask you to describe your symptoms and to keep a bladder diary, recording the volume of fluids you drink and the volume of urine you pass.
- Pelvic exam. During a pelvic exam, your provider examines your external genitals, vagina and cervix and feels your abdomen to assess your internal pelvic organs. Your provider may also examine your anus and rectum.
- Urine test. A sample of your urine is analyzed for signs of a urinary tract infection.
- Cystoscopy. Your provider inserts a thin tube with a tiny camera (cystoscope) through the urethra, showing the lining of your bladder. Your provider may also inject liquid into your bladder to measure your bladder capacity. Your provider may perform this procedure, known as hydrodistention, after you've been numbed with an anesthetic medication to make you more comfortable.
- Biopsy. During cystoscopy under anesthesia, your provider may remove a sample of tissue (biopsy) from the bladder and the urethra for examination under a microscope. This is to check for bladder cancer and other rare causes of bladder pain.
- Urine cytology. Your provider collects a urine sample and examines the cells to help rule out cancer.
- Potassium sensitivity test. Your provider places (instills) two solutions — water and potassium chloride — into your bladder, one at a time. You're asked to rate on a scale of 0 to 5 the pain and urgency you feel after each solution is instilled. If you feel noticeably more pain or urgency with the potassium solution than with the water, your provider may diagnose interstitial cystitis. People with typical bladders can't tell the difference between the two solutions.
Treatment
No simple treatment eliminates the signs and symptoms of interstitial cystitis, and no one treatment works for everyone. You may need to try various treatments or combinations of treatments before you find an approach that relieves your symptoms.
Physical therapy
Working with a physical therapist may relieve pelvic pain associated with muscle tenderness, restrictive connective tissue or muscle abnormalities in your pelvic floor.
Oral medications
Certain medicines that you take by mouth (oral medications) may improve signs and symptoms of interstitial cystitis:
- Nonsteroidal anti-inflammatory drugs, such as ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve), to relieve pain.
- Tricyclic antidepressants, such as amitriptyline or imipramine (Tofranil), to help relax your bladder and block pain.
- Antihistamines, such as loratadine (Claritin, others), which may reduce urinary urgency and frequency and relieve other symptoms.
-
Pentosan polysulfate sodium (Elmiron), which is approved by the Food and Drug Administration specifically for treating interstitial cystitis. How it works is unknown, but it may restore the inner surface of the bladder, which protects the bladder wall from substances in urine that could irritate it. It may take two to four months before you begin to feel pain relief and up to six months to experience a decrease in urinary frequency.
Macular eye disease has been associated with use of this medication in some people. Before starting this treatment, you may need a comprehensive eye exam. You may also need additional eye exams to monitor for eye disease as you continue therapy.
Nerve stimulation
Nerve stimulation techniques include:
-
Transcutaneous electrical nerve stimulation (TENS). With TENS, mild electrical pulses relieve pelvic pain and, in some cases, reduce urinary frequency. TENS may increase blood flow to the bladder. This may strengthen the muscles that help control the bladder or trigger the release of substances that block pain.
Electrical wires placed on your lower back or just above your pubic area deliver electrical pulses — the length of time and frequency of therapy depends on what works best for you.
-
Sacral nerve stimulation. Your sacral nerves are a primary link between the spinal cord and nerves in your bladder. Stimulating these nerves may reduce urinary urgency associated with interstitial cystitis.
With sacral nerve stimulation, a thin wire placed near the sacral nerves sends electrical impulses to your bladder, similar to what a pacemaker does for your heart. If the procedure decreases your symptoms, you may have a permanent device surgically implanted. This procedure doesn't manage pain from interstitial cystitis, but may help to relieve some symptoms of urinary frequency and urgency.

Sacral nerve stimulation device
During sacral nerve stimulation, a surgically implanted device delivers electrical impulses to the nerves that regulate bladder activity. These are called the sacral nerves. The unit is placed under the skin in the lower back, about where the back pocket is on a pair of pants. In this image, the device is shown out of place to allow a better view of the unit.
Bladder distention
Some people notice a temporary improvement in symptoms after cystoscopy with bladder distention. Bladder distention is the stretching of the bladder with water. If you have long-term improvement, the procedure may be repeated.
Botulinum toxin A (Botox) may be injected into the bladder wall during bladder distention. But, this treatment option could lead to not being able to empty your bladder completely when you urinate. You may need to self-catheterize — be able to insert a tube into your own bladder to drain urine — after this treatment.
Medications instilled into the bladder
In bladder instillation, your provider places the prescription medication dimethyl sulfoxide (Rimso-50) into your bladder through a thin, flexible tube (catheter) inserted through the urethra.
The solution sometimes is mixed with other medications, such as a local anesthetic, and remains in your bladder for about 15 minutes. You urinate to expel the solution.
You might receive dimethyl sulfoxide — also called DMSO — treatment weekly for six to eight weeks, and then have maintenance treatments as needed — such as every couple of weeks, for up to one year.
Another approach to bladder instillation uses a solution containing the medications lidocaine, sodium bicarbonate, and either pentosan or heparin.
Surgery
Doctors rarely use surgery to treat interstitial cystitis because removing the bladder doesn't relieve pain and can lead to other complications.
People with severe pain or those whose bladders can hold only very small volumes of urine are possible candidates for surgery, but usually only after other treatments fail and symptoms affect quality of life. Surgical options include:
- Fulguration. This minimally invasive method involves insertion of instruments through the urethra to burn off ulcers that may be present with interstitial cystitis.
- Resection. This is another minimally invasive method that involves insertion of instruments through the urethra to cut around any ulcers.
- Bladder augmentation. In this procedure, a surgeon increases the capacity of your bladder by putting a patch of intestine on the bladder. However, this is performed only in very specific and rare instances. The procedure doesn't eliminate pain and some people need to empty their bladders with a catheter many times a day.
Self care
Some people with interstitial cystitis find symptom relief from these strategies:
Dietary changes. Eliminating or reducing foods in your diet that irritate your bladder may help to relieve the discomfort of interstitial cystitis.
Common bladder irritants — known as the "four Cs" — include: carbonated beverages, caffeine in all forms (including chocolate), citrus products and food containing high concentrations of vitamin C. Consider avoiding similar foods, such as tomatoes, pickled foods, alcohol and spices. Artificial sweeteners may aggravate symptoms in some people.
If you think certain foods may irritate your bladder, try eliminating them from your diet. Reintroduce them one at a time and pay attention to which, if any, worsen symptoms.
Bladder training. Bladder training involves timed urination — going to the toilet according to the clock rather than waiting for the need to go. You start by urinating at set intervals, such as every half-hour — whether you have to go or not. Then you gradually wait longer between bathroom visits.
During bladder training, you may learn to control urinary urges by using relaxation techniques, such as breathing slowly and deeply or distracting yourself with another activity.
These self-care measures also may help:
- Wear loose clothing. Avoid belts or clothes that put pressure on your abdomen.
- Reduce stress. Try methods such as visualization and biofeedback.
- If you smoke, stop. Smoking may worsen any painful condition, and smoking contributes to bladder cancer.
- Exercise. Easy stretching exercises may help reduce interstitial cystitis symptoms.
Alternative medicine
Two complementary and alternative therapies show some promise in treating interstitial cystitis:
- Guided imagery. This type of therapy employs visualization and direct suggestions using imagery to help you imagine healing, with the hope that the body will follow the mind's suggestions.
- Acupuncture. During an acupuncture session, a practitioner places numerous thin needles in your skin at specific points on your body. According to traditional Chinese medicine, precisely placed acupuncture needles relieve pain and other symptoms by rebalancing the flow of life energy. Western medical practitioners tend to believe that acupuncture boosts the activity of your body's natural painkillers.
These treatments have not been well-studied for interstitial cystitis, so be sure to discuss the use of these therapies with your health care provider.
Coping and support
Interstitial cystitis can worsen your quality of life. Support from family and friends is important, but because the condition is a urinary problem, you may find the topic difficult to discuss.
Find a supportive health care provider who is concerned about your quality of life as well as your condition. Seek someone who will work with you to help relieve your urinary frequency, urgency and bladder pain.
You might also benefit from joining a support group. A support group can provide sympathetic listening and useful information. Ask your provider for information on support groups or see the Interstitial Cystitis Association on the web.
Preparing for your appointment
You may be asked to keep a bladder diary for a few days to record information, such as how often you urinate and how much and what kinds of fluid you consume.
For more testing, you may be referred to a specialist in urinary disorders (urologist) or urinary disorders in women (urogynecologist).
What you can do
To get the most from your visit to your health care provider, prepare in advance:
- Write down any symptoms you're experiencing. Include all of your symptoms, even if you don't think they're related.
- Make a list of any medications, vitamins or other supplements you take. Many over-the-counter supplements can irritate the urinary tract. Also note the doses and how often you take the medication or supplements.
- Have a family member or close friend go with you. You may be given a lot of information at your visit, and it can be difficult to remember everything.
- Take a notepad or an electronic device with you. Use it to note important information during your visit.
- Prepare a list of questions to ask. List your most important questions first, in case time runs out.
For interstitial cystitis, some basic questions to ask include:
- Will my symptoms eventually go away?
- What kind of tests might I need?
- Will changing my diet help with my symptoms?
- Could the medicines I take be aggravating my condition?
- Are there any medications that would help ease my symptoms?
- Will I need surgery?
Make sure that you understand what your provider tells you. Don't hesitate to ask your provider to repeat information or to ask follow-up questions for clarification.
What to expect from your provider
Be prepared to answer questions from your provider, such as:
- How often do you feel the urge to urinate with little or no warning?
- Do you feel the urge to urinate immediately after you've urinated?
- Do you ever urinate less than two hours after you finished urinating?
- Do you wake up at night to urinate?
- Do you have pain or burning in your bladder?
- Do you feel pain in your abdomen or pelvis?
- Are you currently sexually active?
- How much do your symptoms bother you?